Introduction
Your hands feel stiff when you wake up. The stiffness lasts more than an hour. Small joints in your fingers ache with a deep, persistent pain. Your doctor runs blood tests and delivers news you weren’t expecting: rheumatoid arthritis.
The diagnosis raises immediate questions. How bad will this get? Will I lose the ability to use my hands? What does the future look like with this condition?
Understanding the four stages of what are the 4 stages of rheumatoid arthritis gives you a roadmap of what might lie ahead. More importantly, it shows you where intervention matters most and how early treatment can dramatically change your trajectory. This guide breaks down each stage of RA progression, explains what happens at each phase, and provides actionable strategies to slow disease advancement.
The good news hiding within a challenging diagnosis: modern treatments have transformed rheumatoid arthritis from an inevitably crippling disease into a manageable chronic condition for most people.
Understanding Rheumatoid Arthritis: The Foundation
Before diving into the stages, you need to understand what drives rheumatoid arthritis in the first place.
What RA Actually Does to Your Body
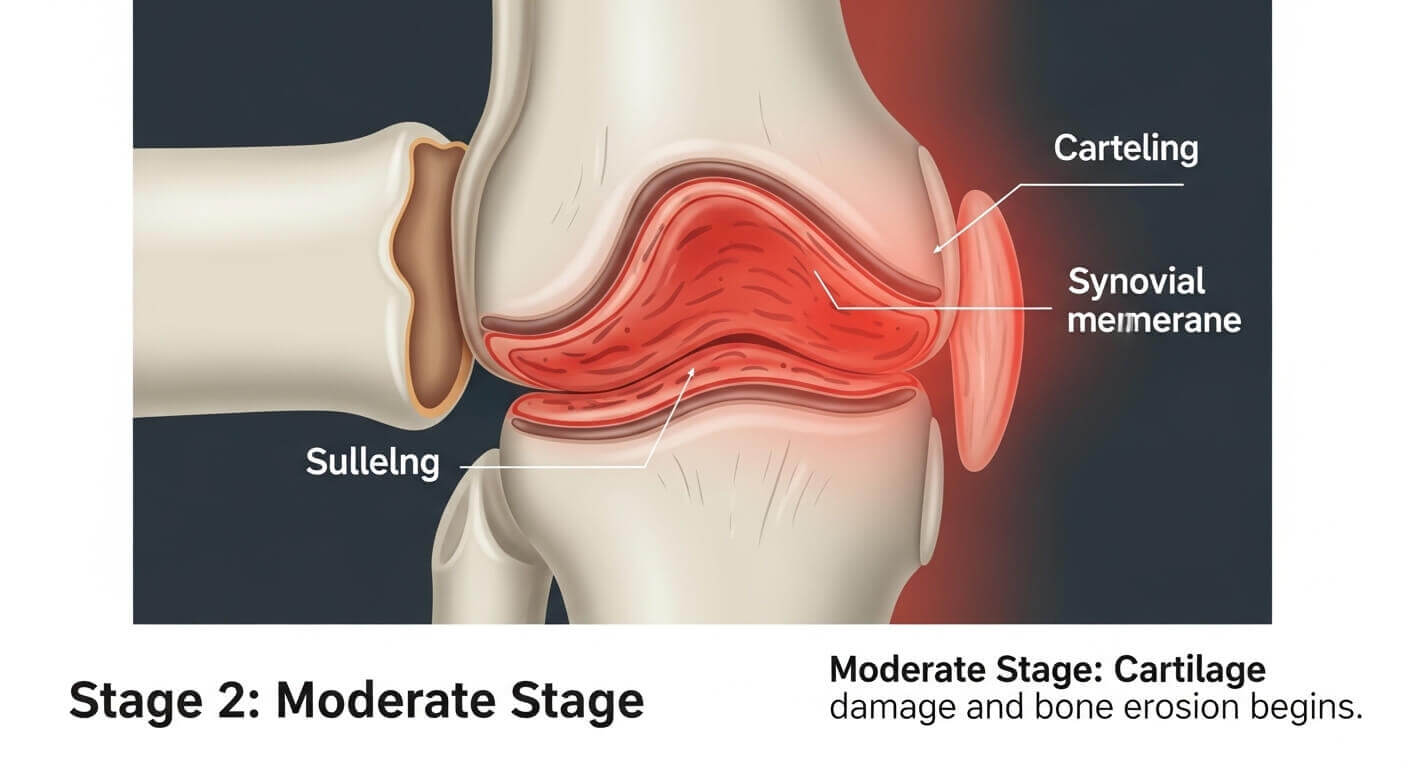
Rheumatoid arthritis is an autoimmune disease where your immune system mistakenly attacks your own body tissues. Specifically, it targets the synovium—the thin membrane lining your joints.
Normally, the synovium produces fluid that lubricates joints and allows smooth movement. When RA strikes, your immune system floods this membrane with inflammatory cells. These cells release chemicals that cause the synovium to swell and thicken.
Over time, this chronic inflammation damages the cartilage cushioning your bones and erodes the bones themselves. Without treatment, joints can become deformed and lose function entirely.
RA typically affects joints symmetrically, meaning if your right wrist is inflamed, your left wrist probably is too. The disease most commonly targets smaller joints first—hands, wrists, feet, and ankles—though it can affect any joint in your body.
Why Stages Matter for Your Treatment
Rheumatologists classify RA into four distinct stages based on the degree of joint damage visible on imaging tests and the severity of symptoms. Each stage requires different treatment approaches and has different prognostic implications.
Catching and treating RA in earlier stages prevents the permanent joint damage that occurs in later stages. Once cartilage erodes or bones fuse, that damage cannot be reversed. Treatment can stop further progression, but can’t repair what’s already lost.
This is why understanding stages matters tremendously. Early intervention during Stage 1 or 2 can prevent you from ever experiencing the severe disability associated with Stage 3 or 4 disease.
Stage 1: Early Rheumatoid Arthritis
The first stage of RA represents the disease at its earliest, most treatable phase. Unfortunately, this stage is also the hardest to diagnose.
What’s Happening in Your Joints
During Stage 1, inflammation begins attacking the synovial lining of your joints. The synovium swells and becomes irritated as your immune system sends inflammatory cells to the area.
Despite this internal inflammation, X-rays taken during Stage 1 typically show no joint damage. The bones themselves haven’t started eroding yet. More sensitive imaging like ultrasound or MRI might show fluid buildup or early inflammation that X-rays miss.
Blood tests may or may not show elevated inflammatory markers like C-reactive protein (CRP) or erythrocyte sedimentation rate (ESR). Antibodies associated with RA—rheumatoid factor and anti-CCP antibodies—can appear in blood years before symptoms develop, though not everyone with RA tests positive for these markers.
Symptoms You Might Experience
Stage 1 symptoms are often subtle and easy to dismiss as general aches or the result of overuse:
Morning stiffness: Joints feel stiff when you first wake up, typically lasting 30 minutes to an hour. This stiffness improves with movement and activity.
Joint pain without obvious swelling: You feel achiness or tenderness in small joints, especially hands, wrists, feet, and ankles. The pain may come and go.
Fatigue: A persistent, overwhelming tiredness that doesn’t improve with rest. This fatigue goes beyond normal tired feelings.
Low-grade fever: Some people run slightly elevated temperatures, usually under 100°F.
Mild swelling: One or a few joints may show slight puffiness, though dramatic swelling is uncommon in Stage 1.
The hallmark of early RA is that symptoms often affect joints on both sides of the body symmetrically. If your right hand hurts, your left probably does too.
Why Early Diagnosis Proves Challenging
Many people brush off Stage 1 symptoms as normal aging, temporary soreness from activities, or minor strains. The symptoms aren’t severe enough to prompt immediate medical attention in most cases.
Even when people do see doctors during Stage 1, diagnosis can be difficult. X-rays look normal. Blood tests might not show classic RA markers. Symptoms overlap with dozens of other conditions.
Rheumatologists rely on a combination of factors to diagnose Stage 1 RA:
- Pattern of joint involvement (symmetric, small joints)
- Morning stiffness lasting over 30 minutes
- Positive blood tests for rheumatoid factor or anti-CCP antibodies
- Elevated inflammatory markers
- Symptoms lasting at least 6 weeks
Treatment Goals for Stage 1
The primary goal during Stage 1 is halting disease progression before permanent damage occurs. Treatment typically includes:
Disease-modifying antirheumatic drugs (DMARDs): Medications like methotrexate work to suppress the overactive immune response causing joint inflammation. Starting DMARDs early provides the best chance of preventing disease progression.
NSAIDs and pain relievers: Medications like ibuprofen or naproxen reduce pain and inflammation but don’t slow disease progression. They provide symptom relief while DMARDs take effect.
Low-dose corticosteroids: Short-term steroid use can quickly reduce inflammation while waiting for DMARDs to work. Doctors typically taper steroids as quickly as possible due to long-term side effects.
Lifestyle modifications: Gentle exercise, physical therapy, stress management, and anti-inflammatory diet changes support medical treatment.
Starting treatment during Stage 1 gives you the best possible outcome. Studies show that people who begin DMARDs within 3 months of symptom onset have better long-term function and less joint damage than those who delay treatment.
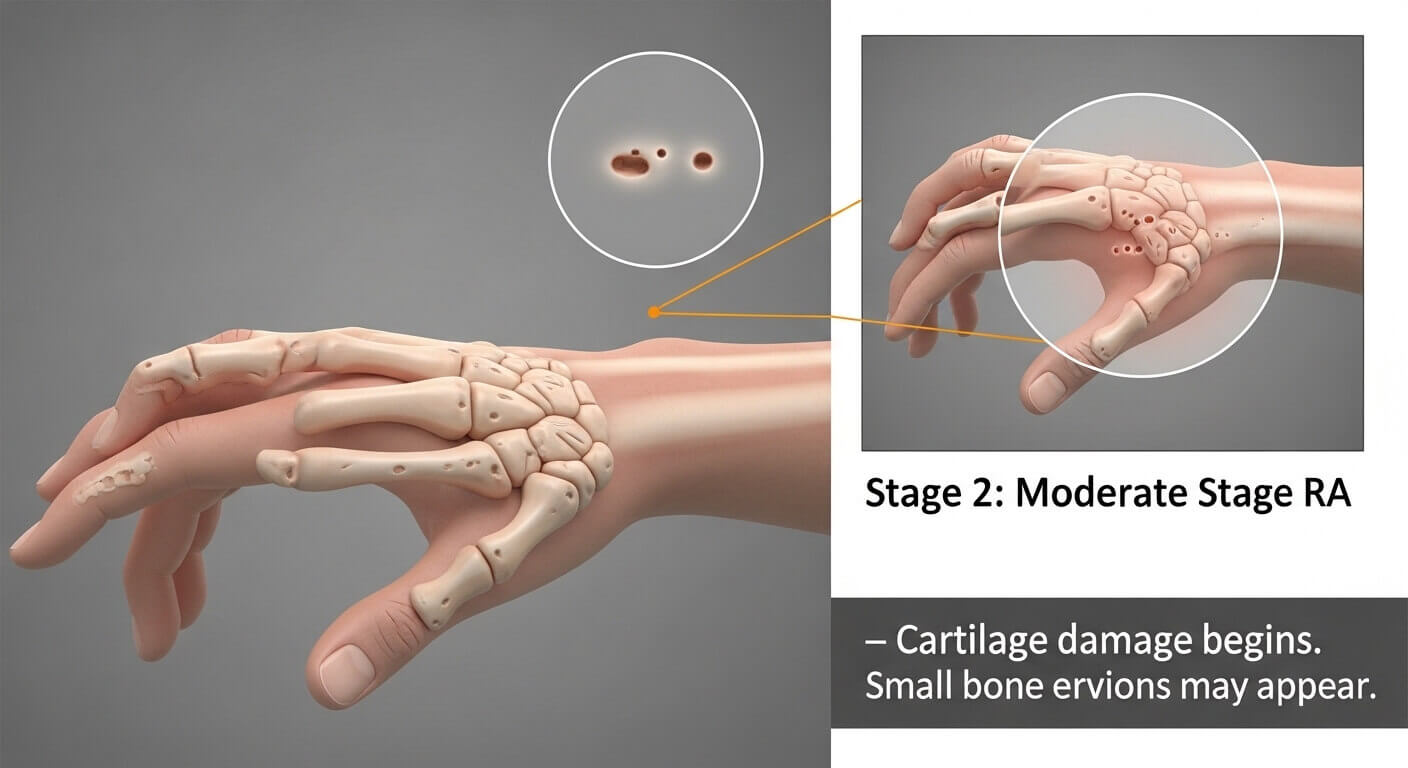
Stage 2: Moderate Rheumatoid Arthritis
Stage 2 marks a transition where inflammation begins causing measurable damage to joint structures.
Joint Changes Become Visible
During Stage 2, inflammation starts destroying cartilage—the smooth, protective tissue covering the ends of bones where they meet in joints. As cartilage breaks down, bones lose their cushioning.
X-rays taken during Stage 2 show:
- Thinning of bones near affected joints (periarticular osteopenia)
- Early bone erosion beneath cartilage surfaces
- Narrowing of joint spaces as cartilage wears away
The damage is real and permanent, though joints still function relatively normally. Range of motion may decrease slightly, and you might notice joints feel stiffer than before.
Symptoms Intensify and Spread
Stage 2 symptoms become harder to ignore and more persistent:
More pronounced joint pain: Pain occurs more frequently and with greater intensity. It may persist throughout the day rather than just mornings.
Noticeable swelling: Joints visibly puff up with fluid. Rings might feel tight or not fit at all. Shoes may need to be sized up.
Extended morning stiffness: Morning stiffness now lasts several hours rather than 30-60 minutes.
Reduced range of motion: You struggle to make a full fist, fully extend fingers, or bend wrists as far as you once could.
Systemic symptoms: RA can now affect other body systems beyond joints. Some people develop rheumatoid nodules—firm lumps under the skin, usually on elbows. Others experience dry eyes, lung inflammation, or anemia.
Bilateral involvement: The symmetric pattern becomes more obvious, with matching joints on both sides affected.
Stage 2 represents the disease spreading from initial affected joints to additional joints throughout the body.
Diagnosis Becomes Clearer
By Stage 2, diagnosis becomes much more straightforward. Blood tests typically show:
- Elevated rheumatoid factor in most (but not all) patients
- Positive anti-CCP antibodies
- High levels of inflammatory markers (CRP, ESR)
X-rays clearly show joint damage that confirms the diagnosis. Some people reach Stage 2 before receiving an RA diagnosis because Stage 1 symptoms were too subtle to prompt testing.
Treatment Intensifies
Stage 2 treatment aims to prevent progression to Stage 3 while managing symptoms:
Combination DMARD therapy: Many rheumatologists add second-line DMARDs to initial methotrexate therapy. Combinations work better than single drugs for many people.
Biologic medications: If traditional DMARDs aren’t controlling disease activity, biologic drugs that target specific immune system components may be added. These include TNF inhibitors, IL-6 inhibitors, and others.
Targeted synthetic DMARDs: Newer oral medications called JAK inhibitors offer another treatment option when methotrexate alone isn’t sufficient.
Physical therapy: Specific exercises maintain joint mobility and strengthen muscles supporting affected joints.
Occupational therapy: Learning joint protection techniques and using assistive devices helps maintain function and independence.
Corticosteroid injections: Injecting steroids directly into severely inflamed joints provides targeted relief.
Aggressive treatment during Stage 2 can still prevent the severe joint deformity characteristic of Stage 3.
Stage 3: Severe Rheumatoid Arthritis
Stage 3 represents severe RA with significant joint damage and functional impairment.
Extensive Joint Destruction
By Stage 3, inflammation has caused substantial damage to both cartilage and bone. X-rays show:
- Significant bone erosion
- Severe joint space narrowing
- Joint deformities visible on imaging
- Possible bone-on-bone contact
Common deformities that develop during Stage 3 include:
Swan neck deformity: Fingers bend abnormally at the middle joints while hyperextending at joints near the fingertips.
Boutonniere deformity: Middle finger joints bend while joints near the fingertips hyperextend.
Ulnar drift: Fingers angle away from the thumb toward the little finger side of the hand.
Hammer toes: Toes bend downward at the middle joints.
These deformities result from ligament and tendon damage combined with bone and cartilage destruction. They significantly impair hand function and make daily tasks difficult.
Functional Limitations Increase
Stage 3 symptoms severely impact quality of life:
Severe, chronic pain: Pain becomes constant rather than intermittent. It interferes with sleep, work, and daily activities.
Major loss of range of motion: Joints move through only a small fraction of their normal range.
Visible joint deformities: Physical changes to joint structure become obvious to others.
Significant functional impairment: Simple tasks like buttoning shirts, opening jars, or walking become challenging or impossible without assistance.
Muscle weakness: Muscles around damaged joints atrophy from disuse and chronic inflammation.
Systemic complications: RA-related problems in other organs may develop, including lung disease, heart problems, or eye inflammation.
Treatment Focuses on Function
While preventing further damage remains important, Stage 3 treatment also emphasizes maintaining whatever function remains:
Aggressive medication management: Multiple DMARDs, biologics, or targeted synthetic DMARDs used in combination.
Pain management specialists: Comprehensive pain control strategies including medications, nerve blocks, and complementary approaches.
Surgical options: Joint replacement surgery for severely damaged hips, knees, or other large joints. Hand surgery can correct some deformities and restore limited function.
Intensive rehabilitation: Physical and occupational therapy to maximize remaining function.
Assistive devices: Splints, braces, canes, walkers, or wheelchairs help maintain mobility and independence.
Mental health support: Chronic pain and disability significantly impact emotional wellbeing. Counseling helps people cope with disease impact.
Reaching Stage 3 doesn’t mean giving up. Many treatment options still exist, and people can maintain reasonable quality of life with proper management.
Stage 4: End-Stage Rheumatoid Arthritis
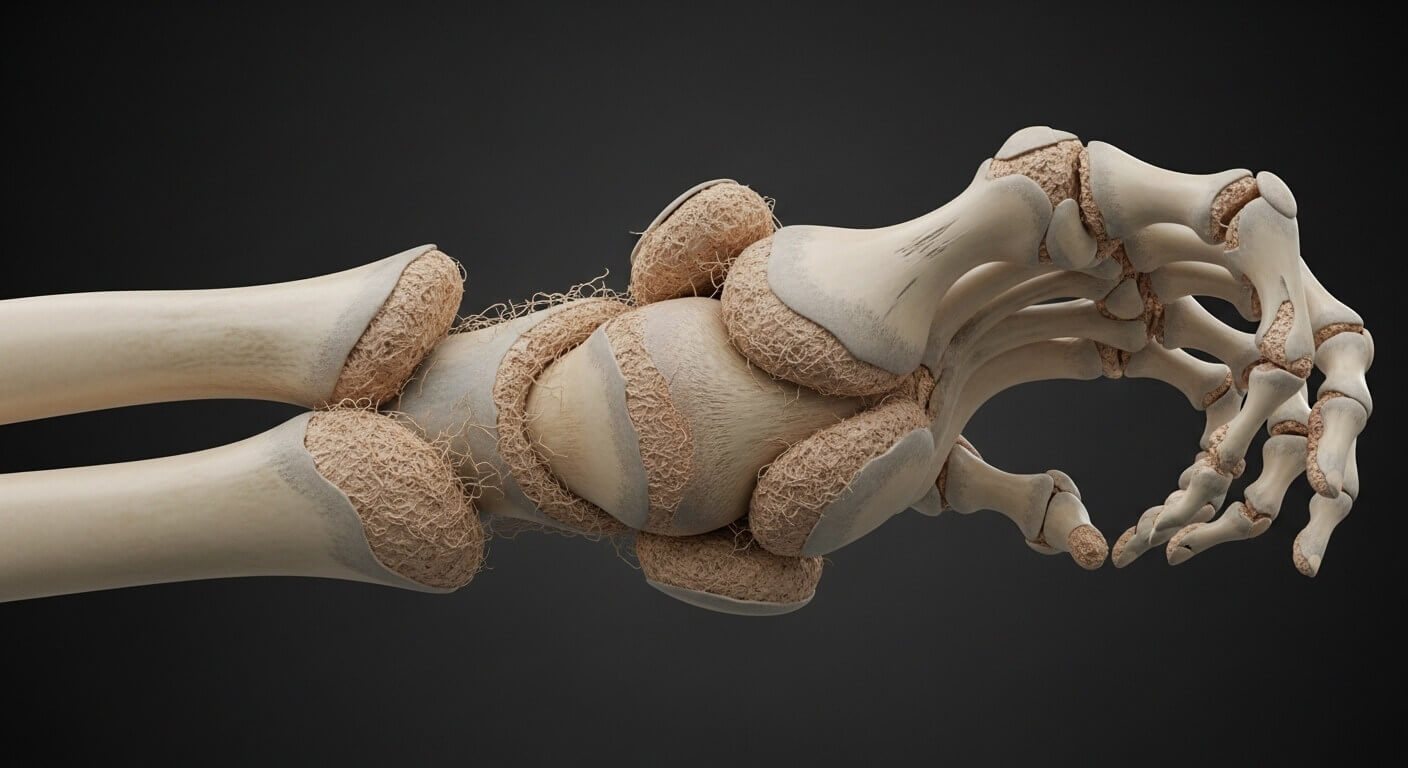
Stage 4 represents the final, most severe stage of RA progression. Thankfully, modern treatment means relatively few people reach this stage today.
Complete Joint Destruction
In Stage 4, inflammation finally subsides, but the damage is done. Joints have deteriorated so severely that they can no longer function:
Ankylosis: Bone grows into joint spaces, causing bones to fuse together. The joint becomes completely immobile.
Total loss of joint function: Affected joints can’t move at all. Hands may freeze in curled positions. Knees may lock in bent or straight positions.
Severe deformity: Joint structure is completely altered from normal anatomy.
X-rays show:
- Complete erosion of cartilage
- Extensive bone destruction
- Joint fusion or complete disintegration
- No recognizable joint space remaining
Life with End-Stage RA
Stage 4 creates profound disability:
Severe, unrelenting pain: Despite inflammation quieting, pain from damaged nerves and bones persists.
Complete loss of mobility in affected joints: Tasks requiring use of fused joints become impossible.
Total dependence on others: Most people need extensive help with basic self-care, eating, and mobility.
High risk of complications: Immobility leads to muscle wasting, blood clots, pressure sores, and other secondary problems.
Significantly reduced quality of life: Physical limitations impact every aspect of daily living.
Treatment Options Are Limited
Treatment for Stage 4 focuses on:
Surgical intervention: Joint replacement surgery offers the only option for restoring function to completely destroyed joints. Not all joints can be replaced, and surgery carries risks especially in people debilitated by advanced RA.
Maximum pain management: Combining multiple pain control strategies to achieve adequate relief.
Maintaining function in unaffected areas: Preserving strength and mobility in joints not yet destroyed.
Preventing complications: Pressure sore prevention, blood clot prevention, infection prevention.
Palliative care: Comprehensive comfort-focused care addressing physical, emotional, and spiritual needs.
The best “treatment” for Stage 4 RA is preventing it from ever happening through early diagnosis and aggressive treatment in earlier stages.
Factors Affecting Disease Progression
RA doesn’t progress at the same rate for everyone. Several factors influence how quickly the disease moves through stages.
Genetic Factors
Certain genetic markers increase RA severity and progression speed. People with specific HLA gene variants tend to have more aggressive disease and greater risk of joint damage.
Rheumatoid factor and anti-CCP antibody levels also predict progression. Higher antibody levels generally correlate with faster disease advancement and worse outcomes.
Smoking Status
Smoking represents one of the strongest modifiable risk factors for RA progression. Smokers with RA experience:
- More severe symptoms
- Faster joint damage progression
- Reduced response to medications
- Higher antibody levels
- Greater risk of lung complications
Quitting smoking improves outcomes significantly. Former smokers have better disease control than current smokers.
Age at Diagnosis
People diagnosed at younger ages often have more aggressive disease that progresses faster. However, older adults with RA face higher complication risks due to aging and other health conditions.
Treatment Timing and Adherence
Nothing affects progression more than when treatment starts and how consistently you take medications:
Early treatment: Starting DMARDs within 3 months of symptom onset provides the best outcomes. The “window of opportunity” for preventing damage exists in early disease.
Consistent medication use: Skipping doses or stopping medications allows disease activity to flare and damage to progress.
Treat-to-target approach: Adjusting medications to achieve low disease activity or remission prevents progression better than just treating symptoms.
Comorbid Conditions
Other health problems influence RA progression:
- Obesity increases inflammation and worsens outcomes
- Diabetes accelerates joint damage
- Cardiovascular disease complicates treatment choices
- Depression reduces medication adherence
Managing these conditions alongside RA improves overall outcomes.
Common Mistakes That Accelerate Progression
Avoiding these errors helps slow RA progression and maintain function.
Mistake 1: Delaying Medical Evaluation
Dismissing early symptoms as “just getting older” or “overdoing it” delays diagnosis and treatment. Every month without treatment during early RA increases the risk of permanent joint damage.
Seek evaluation promptly if you experience:
- Joint pain and swelling lasting more than 2 weeks
- Morning stiffness lasting over 30 minutes
- Symmetric joint symptoms
- Unexplained fatigue
Mistake 2: Stopping Medications When Feeling Better
RA medications work to suppress disease activity, not cure it. When you stop taking them, disease activity returns and progression resumes.
Many people feel so much better on treatment that they assume they don’t need medications anymore. This leads to disease flares and accelerated joint damage.
Continue medications as prescribed, even when you feel well. Discuss any concerns about medications with your rheumatologist rather than stopping on your own.
Mistake 3: Avoiding Physical Activity
Fear of worsening joint damage leads some people to avoid movement entirely. This backfires because:
- Muscles weaken from disuse
- Joints stiffen from lack of movement
- Overall fitness declines
- Weight gain increases joint stress
Appropriate exercise actually helps RA. Low-impact activities like swimming, water aerobics, tai chi, and gentle yoga maintain joint mobility without causing damage.
Mistake 4: Relying Solely on Pain Medication
NSAIDs and pain relievers manage symptoms but don’t stop disease progression. Controlling pain without treating underlying inflammation allows joint damage to continue silently.
Pain relief is important, but disease-modifying treatment must be the foundation of your RA management plan.
Mistake 5: Ignoring Lifestyle Factors
Diet, stress, sleep, and smoking all impact RA progression. Ignoring these factors while only taking medications misses opportunities to slow disease advancement.
Anti-inflammatory eating patterns, stress reduction techniques, adequate sleep, and smoking cessation all support medical treatment.
Expert Tips for Managing RA at Any Stage
Rheumatologists and RA specialists recommend these strategies for optimal disease management.
Build a Strong Healthcare Team
Effective RA management requires multiple specialists:
- Rheumatologist (disease management expert)
- Primary care physician (overall health coordinator)
- Physical therapist (mobility and strength specialist)
- Occupational therapist (function and adaptation expert)
- Mental health professional (emotional support)
- Pharmacist (medication management)
Regular communication among team members ensures coordinated care.
Track Your Symptoms
Keep detailed records of:
- Which joints hurt and when
- Morning stiffness duration
- Fatigue levels
- Medication side effects
- Activities that worsen or improve symptoms
This information helps your rheumatologist fine-tune treatment and catch disease flares early.
Practice Joint Protection
Learn and consistently use techniques that reduce joint stress:
- Use larger, stronger joints when possible (carry with forearms instead of fingers)
- Avoid positions that push joints toward deformity
- Take frequent breaks during activities
- Use assistive devices and adaptive equipment
- Maintain good posture
Prioritize Sleep
Quality sleep reduces inflammation and helps manage pain. Aim for 7-9 hours nightly. Create a sleep-friendly environment and establish consistent bedtime routines.
Manage Stress Effectively
Stress triggers RA flares in many people. Develop healthy stress management strategies:
- Meditation or mindfulness practice
- Deep breathing exercises
- Gentle yoga
- Counseling or therapy
- Support groups
Optimize Your Diet
While no diet cures RA, anti-inflammatory eating patterns may help reduce symptoms:
- Emphasize fruits, vegetables, whole grains, and lean proteins
- Include omega-3 fatty acids from fish or flax
- Limit processed foods, sugar, and saturated fats
- Consider a Mediterranean-style diet
- Stay well-hydrated
Stay Connected
Chronic illness can be isolating. Maintain social connections and consider joining RA support groups where you can share experiences with others who truly understand.
what are the 4 stages of rheumatoid arthritis progresses through four distinct stages, from early inflammation with no visible damage to end-stage disease with complete joint destruction. Understanding these stages empowers you to recognize where you are in the disease process and what lies ahead.
The most critical takeaway: early diagnosis and aggressive treatment during Stages 1 and 2 can prevent you from ever experiencing the severe disability of Stages 3 and 4. Modern disease-modifying medications have transformed RA from an inevitably crippling condition into a manageable chronic disease for most people.
If you’re experiencing symptoms suggestive of RA—morning stiffness, joint pain and swelling, fatigue—seek medical evaluation promptly. Don’t wait to see if symptoms go away on their own. Early intervention provides the best chance for maintaining function and quality of life long-term.
If you’ve already been diagnosed with RA, work closely with your rheumatologist to optimize treatment, adhere to medication regimens, and make lifestyle modifications that support disease control. Regular monitoring allows your doctor to adjust treatment before permanent damage occurs.
The four stages provide a framework for understanding RA progression, but remember: with proper treatment, many people never progress beyond Stage 1 or 2. Your diagnosis doesn’t have to define your future if you take action early and maintain consistent, comprehensive disease management.