Introduction
You wake up one morning and notice something’s wrong in your mouth. Your gums feel puffy and tender. When you brush your teeth, they bleed more than usual. You look in the mirror and see that the tissue around your teeth looks red and inflamed instead of its normal pale pink.
Swollen gums are your body’s alarm system telling you something needs attention. While occasional minor gum swelling might seem like just a nuisance, it often signals underlying problems that require action. Ignoring swollen gums rarely ends well—what starts as mild inflammation can progress to serious gum disease and even tooth loss.
This comprehensive guide walks you through everything you need to know about swollen gums. You’ll learn what causes them, how to recognize warning signs, when to seek professional help, and most importantly, how to treat and prevent this common dental problem. Understanding swollen gums empowers you to protect your oral health and maintain a healthy smile for life.
Understanding Swollen Gums and Why They Matter

Swollen gums, also called gingival swelling or edema, occur when the soft tissue surrounding your teeth becomes enlarged, inflamed, and irritated. This condition affects millions of people and represents one of the most common dental problems dentists encounter.
Healthy gums should appear pale pink in color, firm to the touch, and fit snugly around each tooth. When gums swell, they change dramatically in appearance and feel. They may look redder or even purple, appear shiny and smooth instead of having their normal texture, and feel soft or spongy rather than firm.
The triangular areas of gum tissue between your teeth, called papillae, are often where swelling becomes most noticeable. These areas may puff up and extend higher than normal, sometimes even covering part of your tooth surface.
Research shows that over 42% of adults over age 30 have some form of gum disease, with swollen gums being one of the earliest and most visible symptoms. This statistic matters because gum disease doesn’t stay contained in your mouth. Studies have linked severe gum disease to increased risks of heart disease, diabetes complications, respiratory infections, and even pregnancy complications.
Your gums serve as the foundation supporting your teeth. Just like a house needs a solid foundation, your teeth need healthy gums to remain stable and functional. When gums swell and become diseased, they can no longer support teeth properly, eventually leading to loosening and tooth loss.
Common Causes of Swollen Gums
Understanding what triggers gum swelling helps you address the problem effectively. Multiple factors can cause your gums to become inflamed and puffy.
Gingivitis: The Primary Culprit
Gingivitis represents the most common cause of swollen gums. This early stage of gum disease develops when bacterial plaque accumulates on teeth and along the gumline.
Plaque is a sticky, colorless film of bacteria that constantly forms on your teeth. When you eat foods containing sugars and starches, bacteria in plaque produce acids that irritate gum tissue. Without proper removal through brushing and flossing, plaque hardens into tartar within 24 to 72 hours.
Unlike plaque, tartar cannot be removed with regular brushing and flossing. Only professional dental cleaning can eliminate tartar buildup. As tartar accumulates, it provides more surface area for bacteria to colonize, creating a vicious cycle of increasing inflammation.
Gingivitis symptoms include red, swollen gums that bleed easily when you brush or floss. Many people don’t realize they have gingivitis because symptoms can be quite mild initially. However, without treatment, gingivitis progresses to periodontitis—a more serious form of gum disease that damages the structures supporting your teeth.
Poor Oral Hygiene Habits
Inconsistent or improper oral care creates the perfect environment for swollen gums to develop. When you skip brushing or do it hastily, plaque remains on teeth where it irritates gum tissue and causes inflammation.
Flossing matters just as much as brushing. Your toothbrush can’t reach the tight spaces between teeth where food particles and plaque accumulate. Without regular flossing, these areas become inflamed, causing the papillae between teeth to swell.
Many people brush regularly but use an incorrect technique. Brushing too hard or using a hard-bristle toothbrush can actually damage gum tissue and cause swelling. The goal is gentle but thorough cleaning, not aggressive scrubbing.
Hormonal Changes and Pregnancy
Hormonal fluctuations significantly affect gum health. During puberty, pregnancy, menstruation, and menopause, increased levels of estrogen and progesterone cause more blood to flow to the gums.
This increased blood flow makes gums more sensitive to irritants and more prone to swelling. Your gums essentially overreact to the presence of plaque during these times. Even small amounts of plaque can trigger significant inflammation.
Pregnancy gingivitis is particularly common. The hormonal changes of pregnancy make gum tissue more reactive to bacteria. Some pregnant women develop pregnancy tumors—noncancerous growths on the gums that appear as red, swollen lumps. These typically disappear after delivery but can be uncomfortable during pregnancy.
Women experiencing menopause may notice their gums becoming more sensitive, dry, and prone to inflammation. The decrease in estrogen that occurs during menopause affects oral tissues just as it affects other body systems.
Nutritional Deficiencies
Your diet plays a crucial role in gum health. Deficiencies in certain vitamins can directly cause swollen gums.
Vitamin C deficiency is particularly problematic. This vitamin is essential for maintaining and repairing gum tissue and teeth. Severe vitamin C deficiency causes scurvy, a disease characterized by swollen, bleeding gums, loose teeth, and poor wound healing.
While scurvy is rare in developed countries, mild vitamin C deficiency is more common than you might think, especially among people who don’t eat enough fresh fruits and vegetables. Signs include gums that bleed easily, slow healing of mouth injuries, and increased susceptibility to gum infections.
Vitamin B deficiencies, particularly B12 and folate, can also contribute to gum problems. These vitamins support tissue repair and immune function. When levels drop too low, your body struggles to maintain healthy gum tissue.
Infections: Viral, Bacterial, and Fungal
Various types of infections can cause gum swelling beyond typical gingivitis.
Dental abscesses represent serious bacterial infections that form pockets of pus in or around teeth. An abscess occurs when bacteria reach the inner chamber of a tooth through decay, cracks, or gum disease. The infection causes severe, throbbing pain along with significant gum swelling around the affected tooth.
Abscesses require immediate professional treatment. Without intervention, the infection can spread to other parts of your jaw, face, or even into your bloodstream, creating life-threatening complications.
Viral infections like herpes simplex can cause acute herpetic gingivostomatitis. This condition creates painful sores in the mouth along with red, swollen gums. The herpes virus causes initial infection typically in childhood, then remains dormant in nerve tissue, occasionally reactivating to cause new outbreaks.
Fungal infections, particularly oral thrush caused by Candida yeast overgrowth, can lead to inflamed gums. Thrush appears as white patches on the tongue and inner cheeks but can also affect gum tissue. People with weakened immune systems or those taking certain medications face a higher risk for oral thrush.
Medications That Cause Gum Swelling
Certain prescription medications list gum overgrowth as a side effect. The most common culprits include:
Calcium channel blockers used to treat high blood pressure and heart conditions frequently cause gingival hyperplasia—excessive growth of gum tissue. The gums become enlarged and may partially cover teeth.
Anticonvulsant medications, particularly phenytoin, used to prevent seizures, commonly cause gum swelling. Regular dental cleanings become especially important for people taking these medications.
Immunosuppressant drugs taken after organ transplants or to treat autoimmune diseases can make gums more susceptible to infection and swelling.
If you develop swollen gums after starting a new medication, consult both your physician and dentist. Sometimes switching to an alternative medication eliminates the problem. Other times, more frequent professional cleanings help manage the swelling.
Dental Appliances and Procedures
Braces, dentures, and other oral appliances can contribute to gum swelling when not properly fitted or maintained.
Orthodontic braces make thorough brushing and flossing more challenging. Food particles and plaque easily become trapped around brackets and wires. Without meticulous oral hygiene, gums around braces quickly become inflamed and swollen.
Ill-fitting dentures create constant friction and pressure on gum tissue. This irritation causes inflammation, sores, and swelling where the denture rubs against gums. Dentures should be checked regularly and adjusted as needed because the jawbone naturally changes shape over time.
Dental restorations like crowns and fillings with rough or overhanging edges provide hiding spots for plaque. These areas are difficult to clean properly, leading to localized inflammation and swelling around the restoration.
Mouth Injuries and Trauma
Physical trauma to the gums causes temporary swelling. Common causes include:
Burning your mouth on hot food or beverages creates an area of damaged tissue that swells as part of the healing process. These burns typically resolve within 10 to 14 days.
Cuts or scrapes from sharp foods like chips, pretzels, or hard bread crusts can injure gum tissue. The wound site swells as your body sends healing cells to the area.
Aggressive brushing or improper flossing technique can physically damage gums. Using a sawing motion with floss or snapping it down between teeth can cut into papillae. Brushing with too much force or using a hard-bristled brush wears away gum tissue.
Tobacco Use and Smoking
Smoking and other tobacco use significantly increase your risk of gum disease and swollen gums. Tobacco weakens your immune system’s ability to fight infections, making you more susceptible to bacterial invasion of gum tissue.
Smoking also reduces blood flow to the gums, which impairs healing. This means once inflammation starts, it’s harder for your body to resolve it. Smokers often don’t notice gum problems as early as nonsmokers because reduced blood flow means less bleeding—one of the key warning signs of gum disease.
People who smoke are twice as likely to develop gum disease compared to nonsmokers. They also respond more poorly to treatment and face a higher risk of treatment failure.
Recognizing Symptoms of Swollen Gums
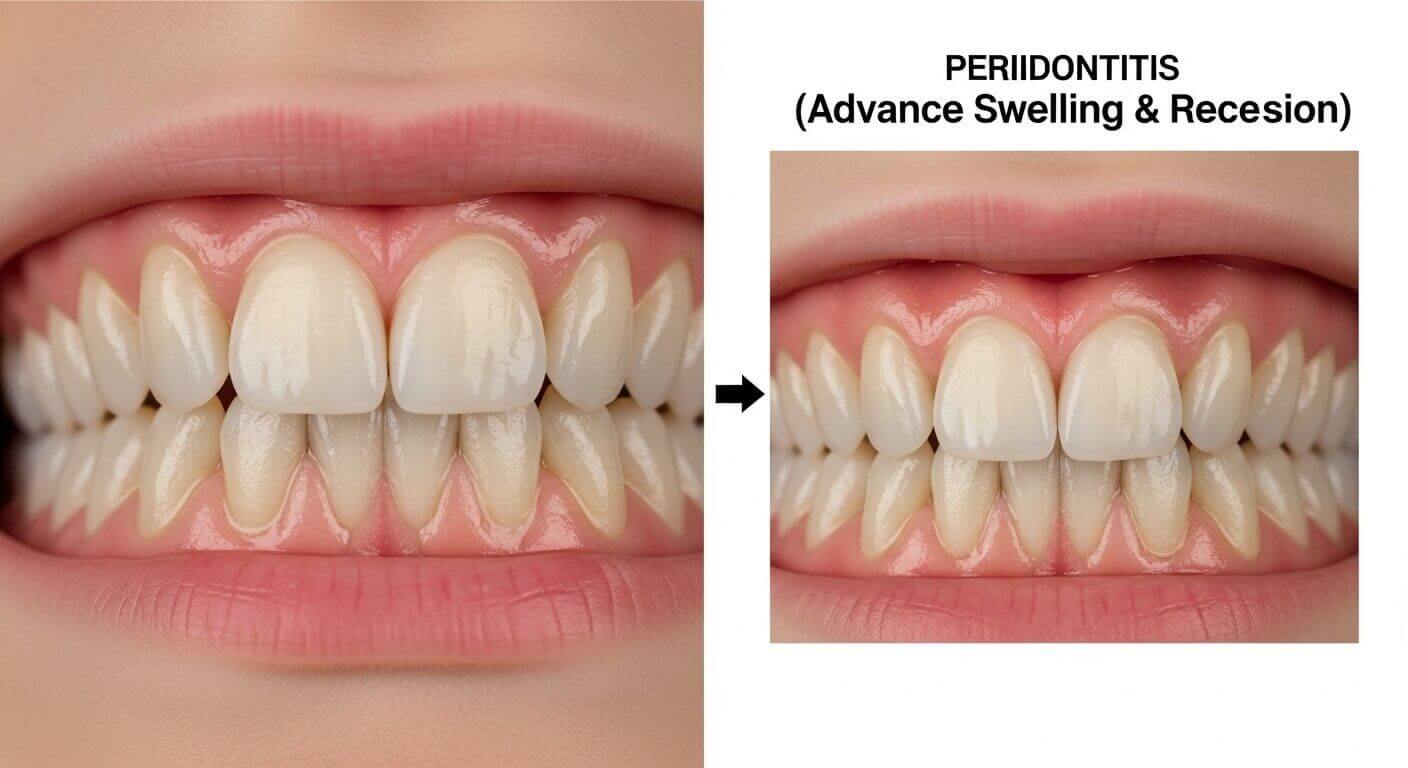
Identifying swollen gums early allows you to take action before minor inflammation progresses to serious disease.
Visual Appearance Changes
Healthy gums have a consistent pale pink color and firm texture with small stippling that looks like orange peel. When gums swell, several visual changes occur.
Color shifts from pink to bright red or even purple. The more intense the inflammation, the redder the gums appear. Purple coloration typically indicates more severe or chronic inflammation.
The tissue looks shiny and smooth instead of having its normal matte, slightly textured appearance. Swollen gums lose their characteristic stippling and become glossy.
Gums may appear to pull away from teeth or recede in advanced cases. Conversely, in early inflammation, gums may look puffier and extend higher up the tooth surface than normal.
Physical Sensations
Swollen gums feel different from healthy tissue. Common sensations include:
Tenderness when touching gums or applying pressure while eating. The inflamed tissue feels sore and sensitive.
Bleeding when brushing, flossing, or eating. Healthy gums shouldn’t bleed from normal oral hygiene activities. Any bleeding indicates inflammation and warrants attention.
A throbbing or aching sensation in the gums, particularly with more severe inflammation or infection. Some people describe a constant dull ache in affected areas.
Functional Problems
Swollen gums can interfere with daily activities:
Difficulty chewing, especially on the side with inflamed gums. The pressure from chewing creates pain in tender, swollen tissue.
Bad breath that persists despite brushing. Bacteria trapped in inflamed gum tissue release foul-smelling compounds.
Changes in how teeth fit together when you bite. Severe swelling can actually alter your bite alignment temporarily.
When to Seek Professional Help
Most cases of mild gum swelling improve with better oral hygiene within a week or two. However, certain symptoms require prompt professional evaluation:
Swelling lasting more than two weeks despite improved oral care indicates a problem that needs professional treatment.
Severe pain or gums that hurt without touching suggest a possible abscess or advanced infection.
A bump or lump on your gums could indicate an abscess, cyst, or other condition requiring diagnosis.
Gums that bleed heavily or continuously need immediate attention.
A fever accompanying gum swelling signals a possible spreading infection.
Difficulty swallowing or breathing represents a medical emergency requiring immediate care.
Treatment Options for Swollen Gums
Treatment approaches vary depending on the underlying cause and severity of gum swelling.
Professional Dental Treatments
A dentist or periodontist can provide several treatments for swollen gums:
Professional cleaning removes plaque and tartar that home care can’t eliminate. Regular cleanings every six months prevent tartar buildup that contributes to inflammation.
Scaling and root planing offer deep cleaning for more advanced cases. This procedure involves cleaning below the gumline to remove bacteria and tartar from root surfaces, then smoothing the roots to help gums reattach to teeth.
Antibiotics may be prescribed for bacterial infections. These come in various forms, including pills, topical gels applied to gum pockets, or antibiotic-impregnated chips placed between teeth and gums.
Surgical intervention becomes necessary in severe periodontitis cases. Procedures like flap surgery access root surfaces for thorough cleaning, while bone and tissue grafts restore structures damaged by advanced disease.
Laser therapy provides a newer treatment option. Dental lasers can remove diseased tissue, reduce bacteria, and promote healing with less discomfort than traditional surgery.
Home Remedies and Self-Care
Several at-home approaches help reduce gum swelling and support healing:
Salt water rinses soothe inflamed gums and reduce bacteria. Mix half a teaspoon of salt in a cup of warm water. Swish for 30 seconds, then spit out. Repeat several times daily.
Warm and cold compresses provide relief. Apply a warm compress to the outside of your face near swollen gums for five minutes, then switch to a cold compress for five minutes. The temperature changes reduce inflammation and numb pain.
Over-the-counter pain relievers like ibuprofen or acetaminophen ease discomfort and reduce inflammation. Follow package directions carefully.
Hydrogen peroxide rinse kills bacteria and reduces plaque. Mix equal parts 3% hydrogen peroxide and water. Swish gently for 30 seconds, then spit out. Don’t swallow. Use no more than twice weekly.
Proper brushing technique matters immensely. Use a soft-bristled brush and gentle circular motions. Brush for two full minutes twice daily, paying special attention to the gumline where plaque accumulates.
Careful flossing removes debris from between teeth without traumatizing gums. Use about 18 inches of floss, wind most around your middle fingers, and gently slide it between teeth using a sawing motion. Curve the floss around each tooth in a C-shape and move it up and down beneath the gumline.
Preventing Swollen Gums
Prevention is always easier and less expensive than treatment. These strategies help keep gums healthy and inflammation-free.
Establish a Solid Oral Hygiene Routine
Brush twice daily for two minutes each time using fluoride toothpaste. Morning brushing removes bacteria that accumulated overnight. Evening brushing eliminates food debris and plaque from the day.
Floss at least once daily, preferably before bedtime. Flossing removes up to 40% of plaque that brushing alone misses.
Use an antibacterial mouthwash to reduce bacteria throughout your mouth. Rinse for 30 seconds after brushing and flossing. Look for mouthwashes with the American Dental Association Seal of Acceptance.
Replace your toothbrush every three to four months or sooner if the bristles become frayed. Worn bristles clean less effectively.
Consider an electric toothbrush. Studies show electric toothbrushes remove more plaque and reduce gingivitis more effectively than manual brushing when used properly.
Visit Your Dentist Regularly
Professional cleanings every six months remove tartar and allow early detection of problems. Some people with a gum disease history need more frequent cleanings every three to four months.
Comprehensive dental exams assess not just teeth but also gums, tongue, and other oral tissues. Early detection of problems allows for simpler, more effective treatment.
Make Smart Dietary Choices
Eat a balanced diet rich in vitamins and minerals essential for gum health. Focus on:
Vitamin C-rich foods like citrus fruits, berries, bell peppers, and broccoli support gum tissue repair and immune function.
Crunchy fruits and vegetables like apples, carrots, and celery naturally clean teeth while you chew and stimulate saliva production.
Calcium and vitamin D from dairy products, fortified foods, and sunlight exposure strengthen teeth and support bone health.
Limit sugary and acidic foods that feed bacteria and weaken tooth enamel. When you do consume them, rinse with water afterward.
Manage Stress Effectively
Chronic stress weakens immune function and makes your body less able to fight infections, including gum disease. Stress also increases inflammation throughout your body, including in your gums.
Practice stress-reduction techniques like meditation, deep breathing exercises, yoga, or regular physical activity. Getting adequate sleep also supports immune function and healing.
Quit Tobacco Products
If you smoke or use other tobacco products, quitting represents the single most important step you can take for gum health. Your dentist can provide resources to help you quit, and many communities offer free cessation programs.
Within just a few weeks of quitting, blood flow to your gums improves. Within months, your risk of gum disease begins to decrease.
Stay Hydrated
Drinking plenty of water throughout the day helps wash away food particles and bacteria. Water also supports saliva production. Saliva neutralizes acids, provides minerals that strengthen teeth, and contains enzymes that fight bacteria.
Aim for at least eight glasses of water daily, more if you’re active or live in a hot climate.
Swollen gums serve as your body’s early warning system, alerting you to problems that need attention. While the condition is extremely common, it’s rarely something you should ignore or simply tolerate.
Most cases of gum swelling stem from inadequate oral hygiene, allowing bacterial plaque to irritate gum tissue. The good news is that gingivitis—the mildest form of gum disease, causing most swollen gums—is completely reversible with improved oral care and professional cleaning.
The key is taking action promptly. Swollen gums that persist for more than a couple of weeks despite better brushing and flossing require professional evaluation. What starts as minor inflammation can progress to serious periodontitis that damages the bone supporting your teeth, eventually leading to tooth loss.
Prevention remains your best strategy. Brushing twice daily, flossing once daily, using mouthwash, and getting professional cleanings every six months prevent most cases of swollen gums before they start. Add a healthy diet, stress management, adequate hydration, and tobacco avoidance, and you’ve created an environment where healthy gums can thrive.
Pay attention to your gums. Notice changes in color, texture, or how they feel. Respond quickly to bleeding or swelling rather than hoping it goes away on its own. Your gums literally hold your teeth in place—they deserve the care and attention that keeps them healthy for a lifetime.